
by Nietling Admin | Feb 25, 2021 | Nietling News
Dr. Nietling was awarded a Certificate of Appreciation from the City of Denison for “Embracing Denison’s vision to restore our magnificent historic buildings in the Downtown District.” Congratulations Dr. Nietling and staff!

by Nietling Admin | Apr 30, 2020 | Nietling News
As we attempt to create a new normal and return to business, Nietling Family Eye Care would like to share what we are doing to ensure the safest environment for all our patients. Our office is taking the following steps including our normal disinfecting/sanitizing protocols in effort to keep everyone healthy.
- The office door is locked at all times. There is no walk-in traffic allowed due to COVID-19 until we may return to full working capacity.
- No walk-in adjustments or repairs allowed. Any optical work must be done by curb side appointment.
- We are scheduling one patient every hour to allow staff proper time to disinfect and sanitize the office.
- We ask that unless a driver is needed for your exam that you come to your appointment alone.
- You will be required to sign a COVID-19 Pandemic Eye Exam and Treatment Consent Form in order to be seen in our office.
- Fever is checked on each patient prior to entering the building.
- Disposable mask are available and we recommend that all patients wear one while in the office.
- Hand sanitizer is available for use by each patient upon entering the office. We ask that you use only as needed, since supplies is limited. This will allow our office to be able to continue to serve you.
- Staff is using hand sanitizer before and after each patient encounter.
- Clipboards, pens, eyeglass frames are being disinfected/sanitized after each patient use.
- Children’s play area items have been reduced to ones we can and do disinfect after each child.
- Magazines have been removed from waiting area.
- Bathrooms are disinfected/sanitized by employees after each use.
- We ask that you do not touch the frames on the board, allow the opticians to bring them to you.
- Pick-up for glasses and other purchases is available through curbside drop off appointments only. Staff will contact you to schedule an appointment for pick up.
We understand that not allowing walk-in traffic may inconvenience some of our patients and we apologize for that. However, in order to maintain a clean safe work and patient care area this will be how we conduct business until further notice. Please contact our offices by phone or email to schedule any of your eye care needs. At the bottom of this article we have provided some links we have found helpful during this time.
CDC Link: https://www.cdc.gov/coronavirus/2019-ncov/index.html
Texas Governor Link: https://gov.texas.gov/news
Grayson County Link: https://www.co.grayson.tx.us/page/covid.home
Collin County Link: https://www.collincountytx.gov/Pages/default.aspx

by Nietling Admin | Jan 23, 2020 | Nietling News
It was an honor to attend the Annual Denison Chamber of Commerce Awards and Gala this evening. Thank you Denison Chamber. Nietling Optical, P.A.- Denison would like to thank the Denison Chamber of Commerce for its recognition of our office as “Small Business of the Year”. We strive to exceed expectations in eye care and give back to our community as we do!!!! Thank you for the many opportunities given to our practice to support and grow in our Texoma area !!



by Nietling Admin | Apr 25, 2019 | Diabetes, Nietling News
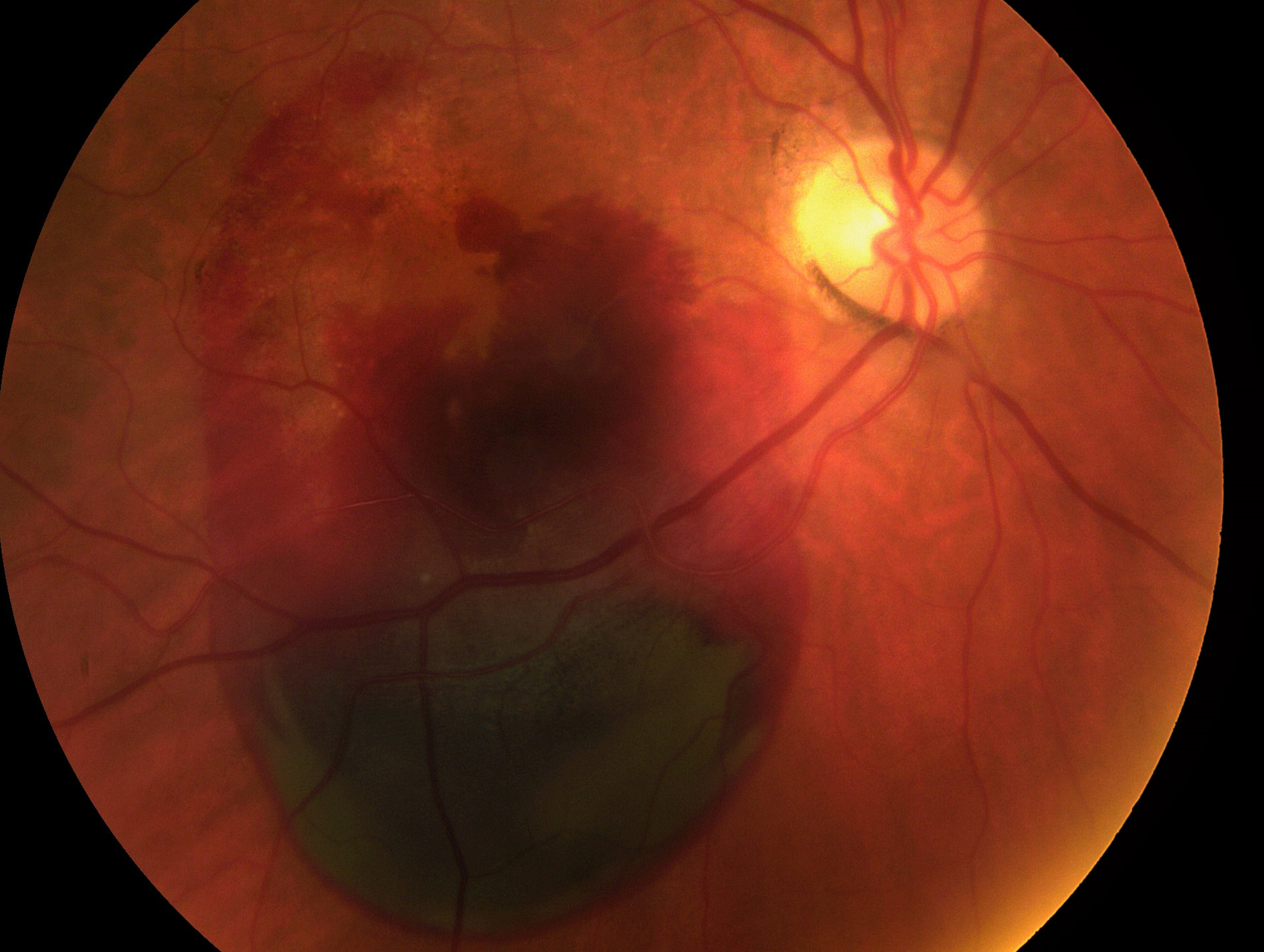
For those of us whom have diabetes, friends that are diabetic or a family history of the disease it is important to know how the disease can affect our vision and eye health. To better understand diabetes in our eyes, first, we must know what is diabetes? Diabetes is a chronic condition that results in too much sugar in the blood. This high blood glucose level over time will weaken and cause changes in the small blood vessels inside your eyes that nourish your retina. These changes cause blood to leak out of the retinal blood vessels; this bleeding can seriously affect your vision, when this occurs, you are then diagnosed with Diabetic Retinopathy. If left untreated Diabetic Retinopathy can cause blindness. Early diagnosis and treatment is an essential key to prevent loss of vision due to Diabetic Retinopathy.
So, how does your eye doctor detect Diabetic Retinopathy? Your optometrist gets to know you, your family history and your personal vision needs through a comprehensive eye examination. It is important to have an annual dilation done by a doctor of optometry if you are a diabetic or have a family history of the medical condition. During this annual in-depth exam, you doctor uses a tool called an ophthalmoscope to look inside your eye through the dilated pupil. This allows your doctor to light up and magnify the inside of the eye. Also, retinal imaging or photographs may be obtained to document and gather even more information about your eye.
What should you look for as a diabetic patient? Beginning stages of Diabetic retinopathy may appear as blurry central or peripheral vision, whereas, you may not notice any symptoms at all. These changes in vision depend on where the bleeding is taking place in your eye. As this ocular disease progresses, you may notice a cloudiness in your vision, blind spots and floaters. Each stage of this disease causes more damage to your eye and the visual symptoms worsen as well. You may experience addition distortion in all ranges of vision and can progress into blindness. When needed there are treatments available that can slow down the progression of diabetic retinopathy. Your eye doctor can recommend a retina specialist for this level of treatment.
As a diabetic patient, the best thing you can do is take steps in your daily living to help prevent the development of Diabetic Retinopathy. By doing so, you are improving your chances to enjoy a lifetime of good vision and health.
Simple Steps for Diabetic Retinopathy Prevention:
- Take your prescribed medication as instructed
- Follow a proper diet
- Exercise regularly
- Have a Comprehensive Dilated Eye Exam done annually
by Nietling Admin | Mar 13, 2019 | Macular Degeneration
How many of us actually know what the macula is or what is does? To better understand the ocular disease Macular Degeneration let’s take a look at this important part of the retina. The macula is the center of the retina and is responsible for providing us with our central vision. Central vision is what we see detail with; it allows us to see the fine print, small objects, color and gives us depth perception. Without our macula 3-D movies could not be appreciated and we would have problems judging distances. So now that we know what it is, why should you be concerned with Macular Degeneration?
Macular Degeneration is a complex eye disease that causes deterioration of the macula cells. Macular Degeneration can be linked to intricate interactions of both environmental and genetic factors. While the exact cause is unknown, evidence suggests that certain key factors such as; sunlight exposure majorly ultraviolet light, high energy blue light exposure from cell phones computer screens, smoking, alcohol use and diets low in carotenoids can increase a person’s likelihood of developing this disease.
There are two forms of Macular Degeneration Wet and Dry. These diseases are considered the leading cause of vision loss in individuals over the age of 50. Case studies also show that they are the leading cause in permanent visual impairment in the United States. Only a comprehensive eye exam can determine if you have Macular Degeneration. Below we’ll list some common symptoms related to Macular Degeneration, but remember these symptoms may also be indicators of other eye health problems. So if you are experiencing any of these please contact a doctor of optometry as soon as possible.
Age Related Macular Degeneration
Signs and Symptoms of Macular Degeneration:
- Gradual loss of the ability to see objects clearly
- Objects appear to be distorted in shape
- Straight line appear wavy or crooked
- Gradual loss of color vision
- A dark or empty area appearing in the center of vision
by Nietling Admin | Nov 18, 2018 | Cataracts, Nietling News
Pretty much everyone has heard of cataracts; either through family, friends or personal experiences, but how much do you know about cataracts? While optometrist may not know precisely what causes cataracts, we can shine the light on key factors that cause changes in our eyes which lead to this ocular condition.
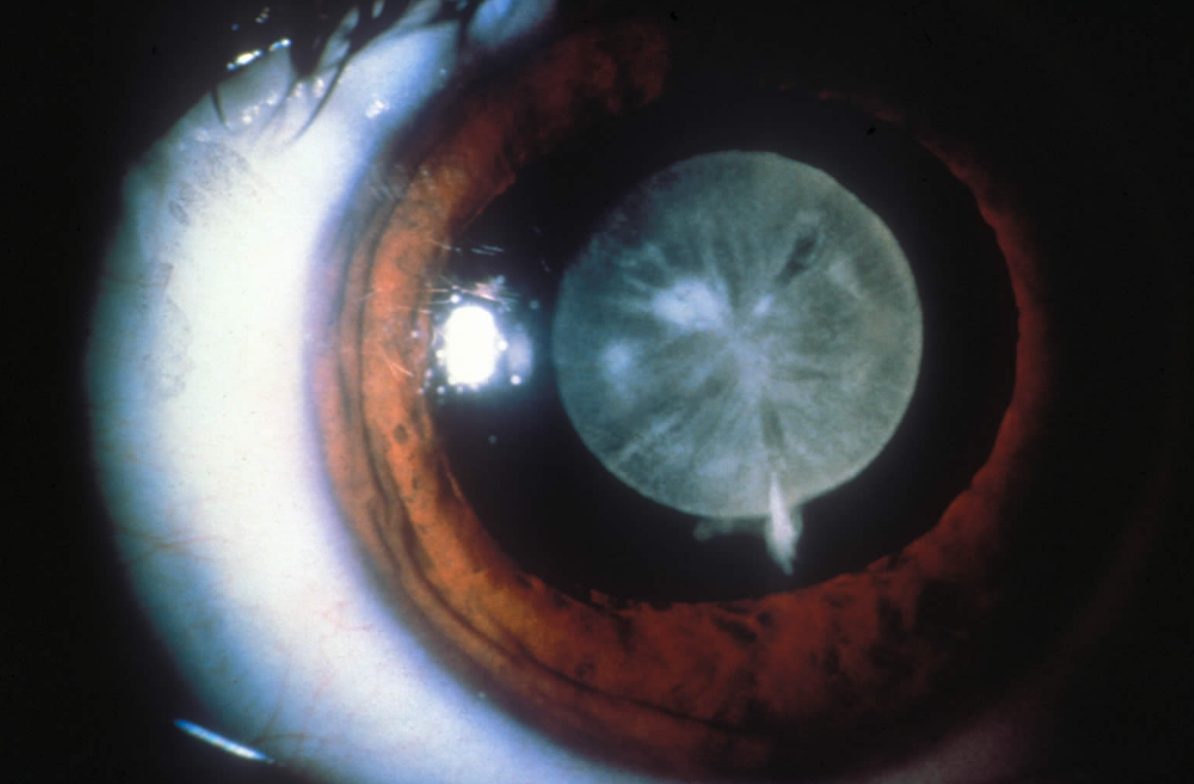
Cataracts by definition are a clouding of the lens in the eye which creates a decrease in vision. As the clouding worsens patients begin to experience symptoms like blurred, foggy, double or ghosting vision. In some cases color vision can also be altered, as well as, sunlight and headlights causing glare problems. Patients will also admit that adjusting to different lighting becomes more difficult (e.g. coming inside from the bright outdoors or going from a dimly lit place to the bright outdoors takes longer to adapt to). 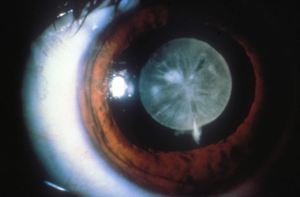
We also know that chemical changes in the lens cause it to get cloudy and advance the stage/severity of cataracts. These chemical changes may be the result of the aging process, heredity, exposure to ultra-violet light, an eye injury, medication (e.g. steroids), disease or a combination of all these factors. While cataracts often appear after the age of fifty, there have been cases found at younger ages, even in babies.
When it comes to the rate of cataract development, well that’s another mystery. This development rate varies from patient to patient. In some instances they can be slow, taking years to disrupt the patient’s visual acuities; while others develop more rapidly within weeks or months from diagnosis. As cataracts develop we often see impairment in the eye’s ability to focus, necessitating a change in glasses or contact lenses to see clearer. Eventually the cloudiness becomes so severe that even changing glasses or contacts will not improve the daily activities. At this point, your eye care professional will need to discuss the need for surgery.
So there you have it, the cloudy truth about cataracts and how they affect your vision.














